Intensive care beds, which cater for critically ill patients, are predicted to represent >30% of all future hospital beds. Around a third of critically ill patients require mechanical ventilation to help them breathe. While a lifesaving intervention, mechanical ventilation increases breathing and heart related complications, decreases quality of life, and costs at least an additional $2000 per patient per day.
During mechanical ventilation the major breathing muscles, namely the diaphragm, abdominal and intercostal muscles, weaken. This weakness increases the length of time that a person has to spend on a mechanical ventilator, which in turn increases rates of hospital re-admissions, illness and death. Interventions that reduce the length of time for which critically ill patients require mechanical ventilation will reduce illness and death, improve the patient’s quality of life and significantly reduce the cost of care.
The application of small electrical pulses to the skin above the abdominal muscles, termed Abdominal Functional Electrical Stimulation (FES), causes the abdominal muscles to contract. We have shown that this improves breathing (McCaughey et al. 2016) and may be a feasible technique to reduce the amount of time for which people with a spinal cord injury require mechanical ventilation (McCaughey et al. 2015).
In this study, we wanted to assess the feasibility of using Abdominal FES with critically ill mechanically ventilated patients. We also wanted to test whether this technique could reduce the length of time these patients required mechanical ventilation for and how long they spent in the intensive care unit.
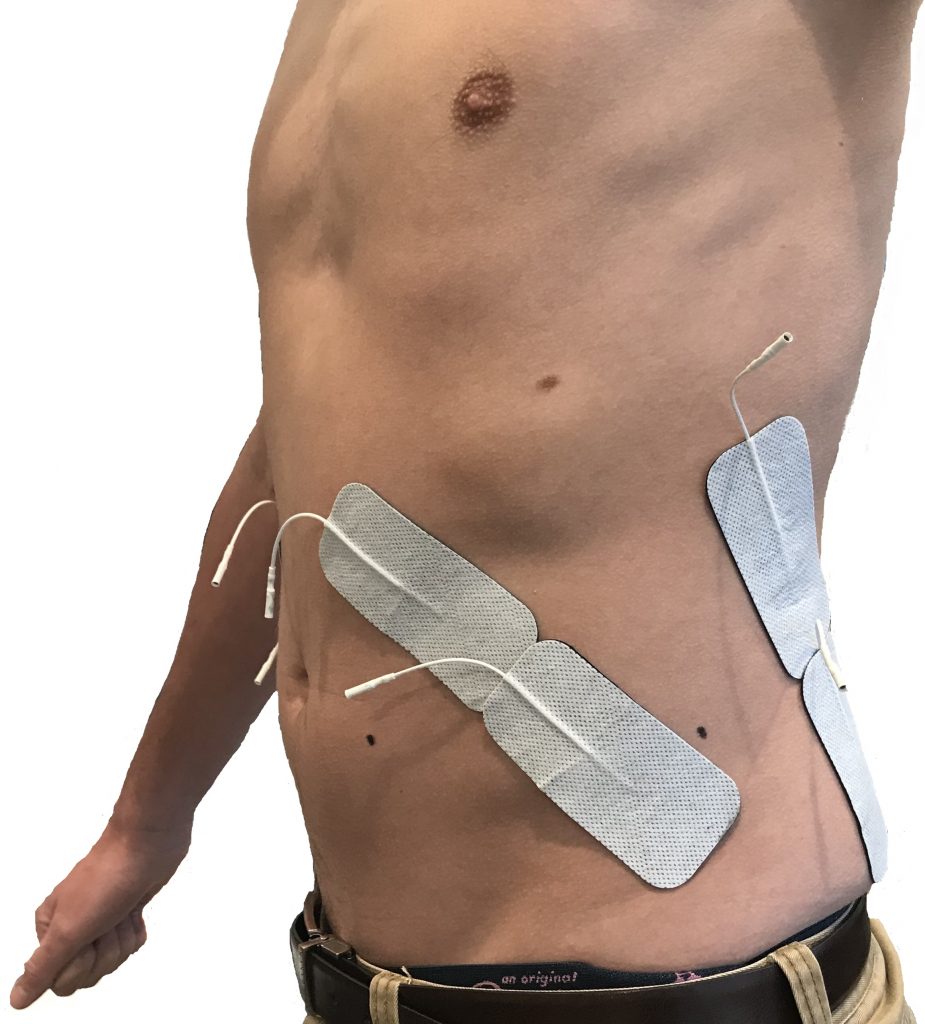
To do this we recruited 20 critically ill participants to this study, 10 of whom received Abdominal FES and 10 of whom received a sham treatment (an inactive treatment or procedure that is intended to mimic as closely as possible a therapy in a clinical trial but does not actually provide the therapy). Both groups received their treatment for one hour per day, 5 days per week, until the participant was discharged from the Intensive Care Unit.
WHAT DID WE FIND?
Of the 20 participants recruited to our study, 6 died in the Intensive Care Unit (2 who got Abdominal FES and 4 who got the sham treatment). We found that the length of time patients required mechanical ventilation for and how long they spent in the intensive care unit was shorter for the patients who got Abdominal FES compared to those who got the sham treatment.
Interestingly, while Abdominal FES causes the abdominal muscles to contract in a similar manner to exercise, at the end of the study there was no difference in the thickness of these muscles between those who got Abdominal FES and those who got the sham. As such, further worker is required to understand how and why Abdominal FES is improving outcomes for these critically ill patients.
SIGNIFICANCE AND IMPLICATIONS
This is the first study to show that Abdominal FES may reduce mechanical ventilation duration and Intensive Care Unit length of stay for people with a critical illness. We hope to validate these results in a larger clinical trial, with a reduction in mechanical ventilation duration and Intensive Care Unit length of stay likely to reduce illness and death, improve the patient’s quality of life, and significantly reduce the cost of care for critically ill patients.
PUBLICATION REFERENCE
McCaughey EJ, Jonkman AH, Boswell-Ruys CL, McBain RA, Bye EA, Hudson AL, Collins DW, Heunks LMA, McLachlan AJ, Gandevia SC, and Butler JE. Abdominal functional electrical stimulation to assist ventilator weaning in critical illness: a double-blinded, randomised, sham-controlled pilot study. Critical Care 23: 261, 2019.
KEY REFERENCES
McCaughey EJ, Borotkanics RJ, Gollee H, Folz RJ, McLachlan AJ. Abdominal functional electrical stimulation to improve respiratory functionafter spinal cord injury: a systematic review and meta-analysis. Spinal Cord 54: 628–639, 2016.
McCaughey EJ, Berry HR, McLean AN, Allan DB, Gollee H. Abdominal functional electrical stimulation to assist ventilator weaning in acute tetraplegia: A cohort study. PLoS One 10: e0128589, 2015.
McCaughey EJ, Boswell-Ruys CL, Hudson AL, Gandevia SC, and Butler JE. Optimal electrode position for abdominal functional electrical stimulation. J Appl Physiol (1985) 125: 1062-1068, 2018
AUTHOR BIO
Dr Euan McCaughey is a Research Fellow at Neuroscience Research Australia and a Conjoint Senior Lecturer at the University of New South Wales. His research focuses on clinical trials of medical devices to improve function after illness or disability. You can follow him on twitter at @EuanMcCaughey.
