Aging is associated with reduced muscle mass and strength. This loss of muscle mass has been termed sarcopenia, meaning “poverty of flesh”. The loss of muscle mass itself is insufficient to account for strength and power decrements during senescence, which has led to the introduction of the term ‘dynapenia’ to denote both the neural and contractile changes contributing to the loss of strength and power with age. Age-related losses of muscle mass, strength and power are critical factors leading to compromised functional mobility in older adults, loss of independence and reduced quality of life.
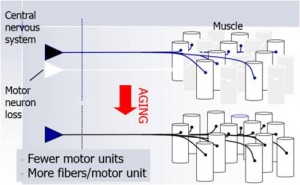
Based on cross-sectional studies, there is a reduction in the number of functioning motor units (the spinal motoneuron and its innervated muscle fibres) after the third decade of life until the 7th decade followed by a rapid decline into very old age. Age-related reductions of 40-60% in the number of functioning motor units occur in several human limb muscles including biceps brachii, extensor digitorum brevis, vastus lateralis, tibialis anterior, soleus and small intrinsic hand muscles when old adults are compared with young adults. This process occurs by a process of motor unit remodelling which, over decades, results in a loss of motoneurons and an enlargement of the surviving motor units. Denervated muscle fibres may atrophy and die, or be reinnervated by nearby motor nerve axon branches. They then adopt the characteristics of the existing fibres in that motor unit (see second figure). Whereas the exact mechanism for this process are not well understood, age-related post-synaptic damage and subsequent muscle fibre atrophy can lead to neuromuscular junction remodelling and impaired neuromuscular transmission stability.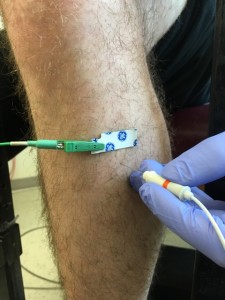
To examine the changes with age, a quantitative estimate of the number of functioning motor units within a muscle can be made electrophysiologically with a technique known as motor unit number estimation (MUNE). There are several different MUNE techniques each with their own limitations. Decomposition-based quantitative electromyography (DQEMG) is one that provides a reliable estimate of the number of functioning motor units in a muscle in both young and old subjects and in patients with neuromuscular diseases. DQEMG also enables the assessment of the stability of neuromuscular transmission.
The benefits of exercise have been recognized for many diseases and for ameliorating the functional declines associated with old age. We were specifically interested in whether exercise provided neuroprotective effects in very old adults. In collaboration with McGill University and the University of Western Ontario in Canada, we tested a unique population of world class master athlete runners. The purpose was to compare motor unit properties of these runners with a cohort of age-matched controls. We wanted to know whether lifelong physical activity influences the preservation and quality of functioning motor units?
WHAT DID WE FIND?
It appears that motor unit numbers and their electrophysiological performance are lower in the age-matched controls compared with the maters athletes. World champion master athletes in their 9th decade of life had more surviving motor units, reduced collateral reinnervation, better preservation of neuromuscular transmission stability and hence better preservation of useable muscle mass as compared with age-matched controls.
Axons of motoneurons extend from the spinal cord (CNS) to the muscle. There each axon divides into a number of axon terminal that form neuromuscular junctions with muscle fibres scattered throughout the muscle.
SIGNIFICANCE AND IMPLICATIONS
Although both groups of older adults are experiencing motor unit remodelling, the master athletes have reduced and more effective reinnervation, indicated by more stable neuromuscular transmission while the age-matched controls presented with more extensive remodelling and less stable neuromuscular transmission. This suggests that maintaining high levels of physical activity has positive effects on motor unit health and performance. Furthermore, the results show greater neuromuscular transmission fidelity across the neuromuscular junction in the master athlete cohort. The presumed better maintenance of motor units in these physically active individuals occurs when motor unit loss is greatest and the loss of muscle mass and strength becomes functionally important; potentially maintaining function and attenuating sarcopenia in this exceptional cohort of older adults. Additionally, with advanced aging, the capacity of motor units to continue sprouting is less effective and this could be driving the reduction in motor unit stability in the age-matched controls. Reinnervation may not be keeping pace with denervation in advanced age.
As this was a small cross-sectional study, the results should be interpreted carefully. We do not know whether these master athletes are genetically advantaged over control subjects. Further studies on the potential neuroprotective effects of exercise in older humans need to identify the role of genetics and the dose of exercise in maintaining neuromuscular structure and function.
PUBLICATION
Power GA, Allen MD, Gilmore KJ, Stashuk DW, Doherty TJ, Hepple RT, Taivassalo T and Rice CL. (2016). Motor unit number and transmission stability in octogenarian world class athletes: can age-related deficits be outrun? J Appl Physiol doi: 10.1152/japplphysiol.00149.2016.
KEY REFERENCES
Campbell MJ, McComas AJ and Petito F. (1973). Physiological changes in ageing muscles. J Neurol Neurosurg Psych 36(2): 174-182.
McNeil CJ, Doherty TJ, Stashusk DW and Rice CL. (2005). Motor unit number estimates in the tibialis anterior muscle of young, old, and very old men. Muscle Nerve 31(4): 461-467.
Power GA, Dalton BH, Behm DG, Doherty TJ, Vandervoort AA, Rice CL. (2010). Motor unit number estimates in masters runners: use it or lose it? Med Sci Sports Exerc. 42(9): 1644-50.
Power GA, Dalton BH, Behm DG, Doherty TJ, Vandervoort AA, Rice CL. (2012). Motor unit survival in life-long runners is muscle-dependent. Med Sci Sports Exerc. 44(7):1235-1242.
Allen MD, Power GA, Filion M, Doherty TJ, Rice CL, Taivassalo T, Hepple RT. (2013). Motor unit number estimates in world-class masters athletes: is 80 the new 60? FASEB J. 27:1150.1. Experimental Biology meeting, Boston, MA. April 20-24.
McKinnon NB, Montero-Odasso M, Doherty TJ. (2015). Motor unit loss is accompanied by decreased peak muscle power in the lower limb of older adults. Exp Geront 70: 111-118.